Inversion or translocation of the chromosome 3, specifically inv(3)(q21q26.2/ t(3;3)(q21;q26.2) are present in 1-2% of acute myeloid leukemia (AML) cases and are classified as a distinct entity in the 2016 WHO classification. Hallmark genetic alterations in this entity include mutations in GATA2 and MECOM. In fact, these rearrangements result in over activation of MECOM due to juxtaposition with a distal GATA2 enhancer. Cytomorphologic phenotypes include anemia, normal to elevated platelets and multilineage dysplasia in a hyperplastic bone marrow (BM). Studies have shown the frequent occurrence of NF1, NRAS and RUNX1 mutations. While proceeding towards our molecularly informed AML subtyping (Awada, Blood 2019;1406), we observed a high occurrence of somatic mutations in the splicing factor SF3B1 in inv(3)/t(3;3) AML. We were particularly intrigued by this observation considering several key aspects of SF3B1 mutations in the context of MDS. For instance, SF3B1 mutations are highly associated with clear phenotypic and morphologic features and carry favorable prognosis in MDS. These mutations are often found in patients carrying less deleterious abnormalities [e.g., del(5q)] and their founder clonal nature has been uncovered through experimental studies. Recent studies unveiled the occurrence of SF3B1 mutations in de novo AML and low complete remission rate when combined with other mutations (e.g., DNMT3A).
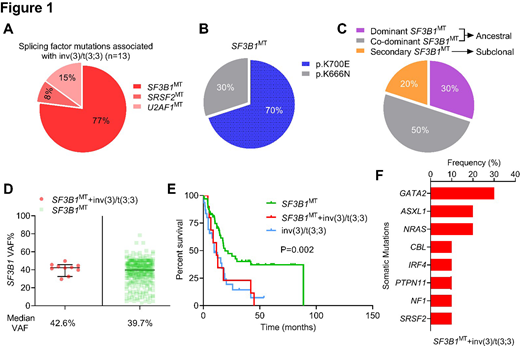
To investigate whether SF3B1 mutations were unequivocally frequent in inv(3)/t(3;3) AML compared to other splicing factor mutations, we moved forward in dissecting the clinical, morphologic and molecular profiles of these cases. We analyzed results from whole exome sequencing and targeted deep sequencing from the Cleveland Clinic and publicly available data of AML with inv(3)/t(3;3) (de novo AML, n=32; secondary AML from antecedent myeloid neoplasms, n=11; t-AML, n=1). In our cohort, mutations in the most common components of the RNA splicing machinery (SF3B1, SRSF2, U2AF1, ZRSR2) were observed in 27% (n=12) of the patients. Among splicing factor mutations, SF3B1 was the most mutated gene (77%; 10/13 total mutations); 7 cases had inv(3) and 3 had t(3;3). Mutations were observed at canonical sites: K700E (70%) and K666N (30%) with no difference compared to the hotspots observed in MDS. Sixty% of patients were female. Median age was 61 years (range, 36-73). Anemia was present in 50%, leukopenia in 10% and thrombocytopenia in 50% of the patients. For 40% of the cases, BM smears for iron staining was available and showed absence of ringed sideroblasts. Complex karyotype (CK) was present in 20% of the patients; -7/del(7q) was present as the only cytogenetic abnormality in 30% or with CK in 10% pf the cases. Variant allele frequency (VAF) of SF3B1mutations in inv(3)/t(3;3) was not different than the those without inv(3)/t(3;3) (42% vs 40%). Survival analysis was performed in 3 subgroups: SF3B1MT AML (n=70), SF3B1MT AML + inv(3)/t(3;3) (n=10), AML + inv(3)/t(3;3) (n=34). SF3B1MT AML + inv(3)/t(3;3) and AML + inv(3)/t(3;3) had similar OS (11.7 vs 9.7 months) which was shorter than the that of SF3B1MT AML without any inv(3)/t(3;3) (19.4 months, P=0.002) suggesting that SF3B1MT in the context of inv(3)/t(3;3) might hold a different prognostic significance strongly due to the presence of inv(3)/t(3;3). Given this observation, we delved into the clonal diversity of SF3B1 mutations and its co-occurrence with other molecular mutations. Comparison of VAFs showed that SF3B1 mutations in relation to other mutations were dominant/founder in 30%, secondary/subclonal in 20% while co-dominant to another gene (VAF differences <5%) in 50% of the cases. The most common co-dominant gene mutation was GATA2 (60%, 3/5). Top mutations by frequency were in GATA2 (30%), ASXL1 (20%) and NRAS (20%). Hemizygous GATA2 mutations were detected in 15% of SF3B1MT AML + inv(3)/t(3;3). In our cohort, other RAS gene mutations were detected in 10% of the patients each, including CBL, NF1 and PTPN11). One SF3B1MT AML + inv(3)/t(3;3) case also harbored a SRSF2 mutation with a parallel median VAF of 40% and 41%, respectively. The results of our study are summarized in Fig. 1.
In sum, we describe that SF3B1 mutations occur in combination with inv(3)/t(3;3) in AML and might represent a subclass of this entity in which lesions in SF3B1 gene could potentially hide a cryptic association between splicing abnormalities and disease phenotypes.
Maciejewski:Alexion, BMS: Speakers Bureau; Novartis, Roche: Consultancy, Honoraria.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal